May 24, 2026 BACKGROUND: The primary way that the United States government, working with nonprofits, has fought hunger and malnutrition around the world has been through the U.S. Food for Peace program (originally Public Law 480, or PL 480), which began in 1954 and was expanded by President Kennedy in 1961, at which time it took on the name Food for Peace (FFP). Over seven decades, it has reached roughly 4 billion people in 150 countries through a mix of emergency relief and longer‑term development projects. Annual funding has typically ranged from $1.2–2 billion in recent years for the core Title II program (the main grant‑based humanitarian component), though overall international food assistance outlays have averaged $2–2.6 billion, fluctuating with global needs.
The structure and flow of resources for FFP begin with Congress, where appropriations come through agriculture and foreign operations bills. In its early history, most FFP aid went to “development,” but over time the balance has shifted toward emergencies. The main food commodities provided by the United States have been wheat, rice, sorghum, corn‑soy blends, beans, peas, lentils, vegetable oil, and ready‑to‑use supplemental foods. These are purchased competitively from U.S. farmers and producers and often bagged on ocean freighters bound for Africa, Asia, Latin America, and the Middle East.
RECENT ADMINISRATIVE SHIFTS: After the Trump Administration dissolved USAID in 2025, FFP planning and administration moved temporarily to the State Department and then, in late 2025, to the U.S. Department of Agriculture, with a strong “America First” focus on buying American‑grown foods. In December 2025, USDA and the U.S. Department of State signed an interagency agreement for USDA to take over FFP. USDA has long supervised other in‑kind international food aid programs, including the school‑feeding‑focused McGovern‑Dole Food for Education and the development‑focused Food for Progress (FFPr) programs, each delivered via partnerships with NGOs and the U.N. World Food Programme.
For many months it had been unclear how USDA would redesign FFP, how it would work with other organizations to deliver aid, and where. Then, in early May 2026, USDA announced a $350 million allocation of foods to WFP. In response, U.S. Wheat Associates announced that it “welcomes the announcement of the award of 20,000 metric tons (MT) (735,000 bushels) for emergency feeding programs under the U.S. Department of Agriculture’s (USDA) administration of the FFP program.”
NEW OFFERINGS
The new May 2026 Notice of Funding Opportunities published by USDA for NGO proposals sets out three reforms USDA has applied to the inherited portfolio:
- *-100% U.S. origin for every commodity procured.
- *-Strict traceability of every taxpayer dollar to guard against fraud, waste, and diversion.
- *-“Offboarding and graduating” criteria, so that Title II funding “prioritizes emergency and in‑need geographies rather than forever‑aid countries.”
At present, the geographic scope has narrowed. NGO applications can only be submitted for seven countries: Democratic Republic of the Congo, El Salvador, Ethiopia, Guatemala, Haiti, Kenya, and Rwanda—a notable contraction from the broader Title II caseload USAID historically managed. Award sizes range from $20 million to $200 million, with USDA anticipating seven to fourteen awards out of $357 million in available federal funding, and a performance period of 18 to 24 months. The application submission deadline is June 12, 2026. Eligible applicants include public or private organizations, including intergovernmental organizations, language that explicitly keeps WFP and similar multilateral partners involved, while foreign governments are excluded.
With the large‑scale defunding of U.S. NGOs and other aid partners in 2025,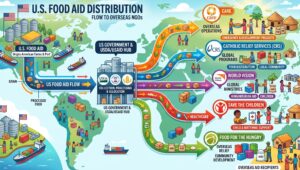 intense competition for these new FFP program awards is expected. NGOs such as CARE, CRS, World Vision, Mercy Corps, Save the Children and Action Against Hunger are expected to be seeking FFP grants.
intense competition for these new FFP program awards is expected. NGOs such as CARE, CRS, World Vision, Mercy Corps, Save the Children and Action Against Hunger are expected to be seeking FFP grants.
At the same time, USDA is layering the program on top of its existing Food for Progress (FFPr) framework. Separate from Title II FFP, the new FY26 Food for Progress solicitation to NGOs—released last week, closing July 6, 2026, with awards expected by late September—makes up to $226 million available across seven countries: Bangladesh, Bolivia, Ecuador, Morocco, Philippines, Sri Lanka, and Thailand, with awards of $28–35 million over four‑to‑five‑year performance periods. Food for Progress operates on a monetization model authorized under the Food Security Act of 1985 (7 U.S.C. § 1736o) in which the USDA buys U.S. commodities domestically and ships them overseas, the NGO sells them in emerging markets, and the NGO uses the proceeds to fund agricultural development. Monetization used to be standard as well for FFP programs particularly in the 1990s.
Both of these competitions for bids are concurrent with USDA funding opportunities for school feeding (McGovern‑Dole).
See also: USDA: https://www.fas.usda.gov/programs/food-peace
and: https://www.devex.com/news/house-locks-food-for-peace-into-usda-with-50-commodity-requirement-112420
A primer from the Congressional Research Service here






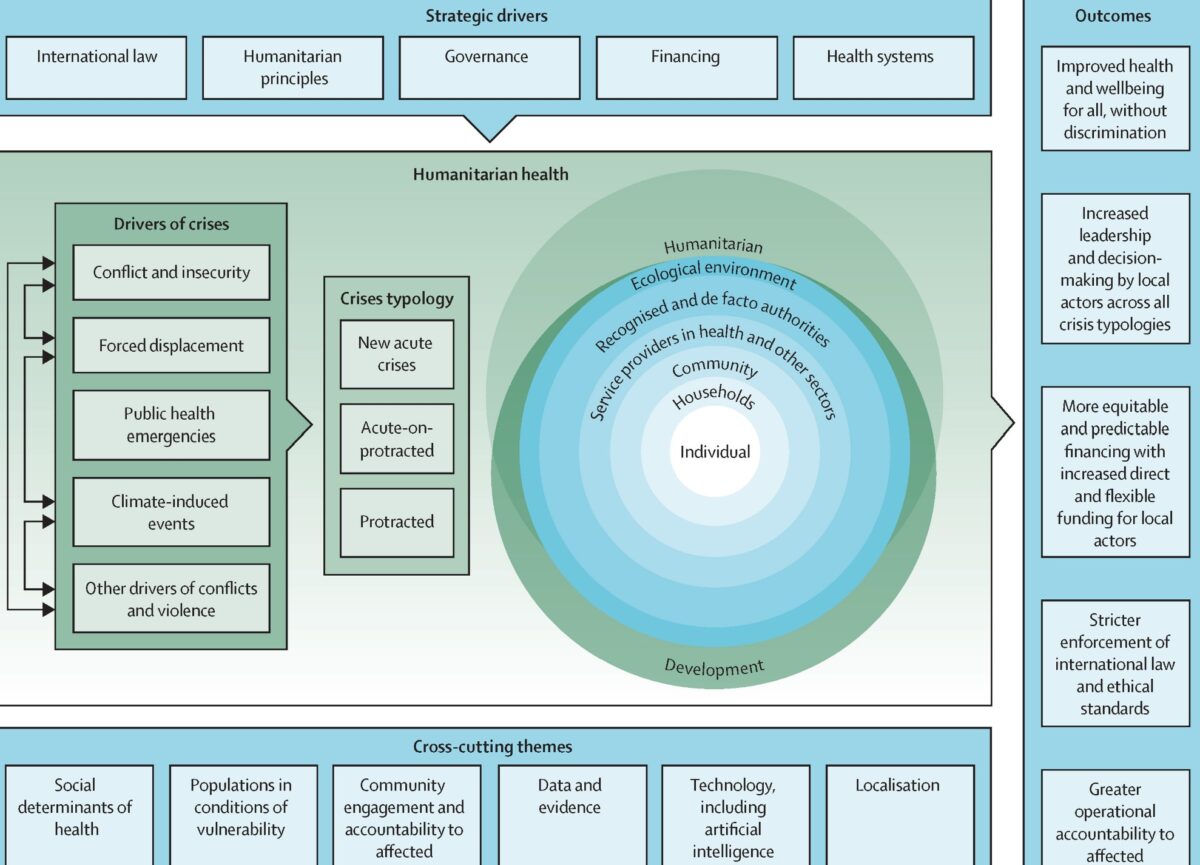

 systems.” And then concludes: “Creating an effective community-centred humanitarian system that provides a more just, robust, and sustainable future needs to be managed carefully and responsibly. “
systems.” And then concludes: “Creating an effective community-centred humanitarian system that provides a more just, robust, and sustainable future needs to be managed carefully and responsibly. “ communities in need.
communities in need.



 listened patiently and always with profound empathy and genuine positive interest that drew so many of us to seek his counsel and company…. Wherever he went, he wanted to know where people were from, what their lives were like, how history had shaped their journeys. Charlie read voraciously and liked nothing more than chatting about a great book, a fascinating trip somewhere, or encounters he had had with interesting people. The world never ceased to fascinate. … he was a very free person. His mind could focus on the curious, the beautiful, the uncanny.”
listened patiently and always with profound empathy and genuine positive interest that drew so many of us to seek his counsel and company…. Wherever he went, he wanted to know where people were from, what their lives were like, how history had shaped their journeys. Charlie read voraciously and liked nothing more than chatting about a great book, a fascinating trip somewhere, or encounters he had had with interesting people. The world never ceased to fascinate. … he was a very free person. His mind could focus on the curious, the beautiful, the uncanny.”

 a no-hitter playing for the Baltimore Black Sox, with a career 3.5 ERA over 15 competitive seasons.
a no-hitter playing for the Baltimore Black Sox, with a career 3.5 ERA over 15 competitive seasons.



 Diseases Hospital in Dhaka admitted 560 suspected measles cases in the first three months of 2026, compared to just 69 cases in all of 2025. (
Diseases Hospital in Dhaka admitted 560 suspected measles cases in the first three months of 2026, compared to just 69 cases in all of 2025. (

 would later become UNHCR), where he continued to use his fame as a polar explorer and diplomat to call attention to the victims of famine and genocide in Russia, Ukraine, and Armenia. In 1922, Nansen received the Nobel Peace Prize for his tireless work for refugees in Europe after the war.
would later become UNHCR), where he continued to use his fame as a polar explorer and diplomat to call attention to the victims of famine and genocide in Russia, Ukraine, and Armenia. In 1922, Nansen received the Nobel Peace Prize for his tireless work for refugees in Europe after the war.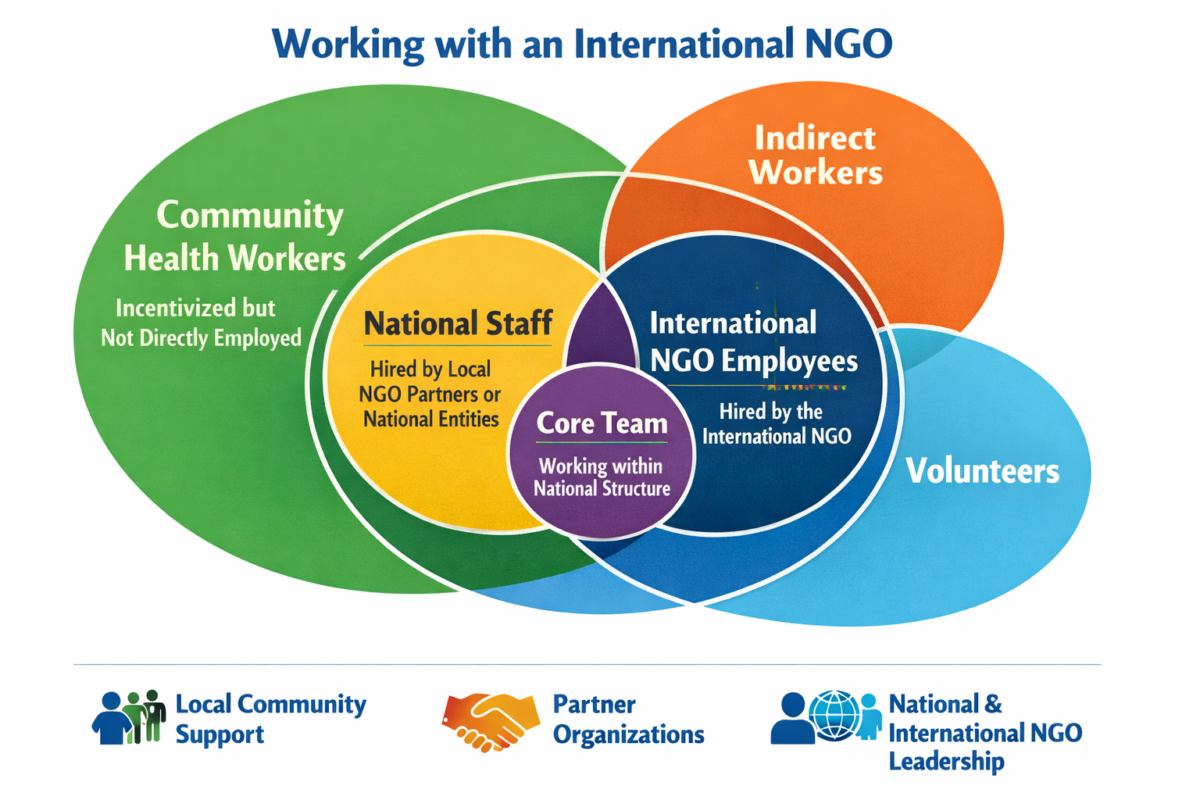
 remain siloed within organizational systems and responsibilities, weakening crisis response.
remain siloed within organizational systems and responsibilities, weakening crisis response.


 they’re able to invest in the business. And so we see better impacts — both in terms of increasing income, savings, and nutrition….We’ve been rolling out a program called DreamSave, which is a digital bookkeeping application at the savings group level that runs on a smartphone. That’s been really well received and has had some positive impacts on the actual savings of the savings groups.”
they’re able to invest in the business. And so we see better impacts — both in terms of increasing income, savings, and nutrition….We’ve been rolling out a program called DreamSave, which is a digital bookkeeping application at the savings group level that runs on a smartphone. That’s been really well received and has had some positive impacts on the actual savings of the savings groups.”

 – the Struggle For Food and Dignity in Recent Humanitarian Crises” was a 2007-08 Hunger Watch Report by Action Against Hunger. It
– the Struggle For Food and Dignity in Recent Humanitarian Crises” was a 2007-08 Hunger Watch Report by Action Against Hunger. It 